Colossus Of Care: New Parkland Hospital
At 2.1 million square feet and an anticipated 30,000 people passing through its doors each day, Dallas County’s New Parkland Hospital, opening Aug. 20, is a monumental achievement in more ways than one.
Since its inception in 2008, the $1.33 billion, 862-bed facility remained the nation’s largest healthcare construction project in progress and, now completed, today stands among the largest public hospitals in the U.S.—an outlier to industry norms that would define a building half its size as a “megaproject.” However, it isn’t just square footage that’s set Parkland apart.
With two architects, four general contractors, countless stakeholders, hefty public funding, persistent media scrutiny, and a directive to create a hospital of choice regardless of its safety-net designation—all planned, designed, and built at the same time healthcare reform was being realized—the completion of Parkland was, in short, no easy task.
And although it’s unlikely that many will follow in its particular footsteps—or footprint—the story of Parkland started just like so many others: The county needed a new hospital to replace its antiquated building.
From scratch
Built in 1954, the existing Parkland Memorial Hospital’s 1 million square feet houses 720 patient rooms, of which only about 30 percent are private and even fewer have showers, with double-loaded 8-foot corridors and an aging infrastructure that left few options for renovation or reuse. Although a replacement was first proposed in the mid-‘90s, it took about a decade of thorough data analysis (building assessments, volume projections) to get the project off the ground.
A $747 million bond referendum was placed on the county ballot in November 2008 and approved by 82 percent of voters. That sum was just a piece of the overall funding puzzle, which also includes $150 million in philanthropic support, $40 million in investment income, and $392 million in hospital reserves.
Parkland already owned a brownfield site just across from the existing hospital on Harry Hines Boulevard with enough acreage for the replacement.
Parkland brought on Blue Cottage Consulting to develop the program even before the bond issue was passed, so when the design team joint venture of HDR + Corgan was brought on board in 2009, with a program but no master plan (a previous plan had been scrapped for various reasons), it was handed a unique scenario. “Usually you develop the master plan and the program, and the master plan dictates the placement of the building and you design the building within that framework,” says Hank Adams, design manager for the project and director of healthcare for HDR (Dallas).
Instead, the team had the luxury—albeit an intimidating one, Adams describes—to start with a rare blank slate and create a building that’s truly assimilated within its site, thanks to the opportunity to simultaneously design the building and master plan the campus. “We learned that [doing both] can be done and that you can actually get a more integrated and better-designed solution because you can manipulate the site and manipulate the design of the building so that they’re both completely coordinated together,” Adams says.
During the process, HDR led the clinical planning and building organization, with Corgan managing logistics.
Soon, several major themes emerged, starting with the concept of connectivity. With public transit (bus and rail) stations on the site as well as a regional train station across the street, the campus could be designed in a way that best took advantage of those access points and created a building scale that embraced the community at a pedestrian level while also providing direct access to neighboring buildings in the Southwestern Medical District. Another hallmark of the plan was the idea of a “hospital in a park,” which influenced the creation of linear parks, gardens, and views and sightlines from within the building back out onto the campus.
Ownership also requested the creation of a modern icon for Dallas and one that was thoroughly of Parkland. “They wanted something that when you looked at it, you knew it was Parkland and you knew what it stood for,” says Robyn Roelofs, interior design lead on the project and senior interior designer at HDR (Dallas).
Taking shape
And while an icon is indeed what Parkland got in the end, it wasn’t necessarily the request for one that dictated the striking exterior with its can’t-miss 60-foot cantilever, bridged buildings, and keyhole opening; it was actually the program.
Blue Cottage stayed on board during schematic design to help with operational flows and adjacencies that had been plotted out through numerous simulation exercises and agreed upon by hospital leadership, with HDR + Corgan performing program validation. One of the major pieces of the effort was to answer a call from the surgical and anesthesiology teams to have surgery, the post-anesthesia care unit, and labor and delivery located on a single floor—a move that established a massive 160,000-square-foot floor plate—with other diagnostic and treatment functions stacked vertically within that floor plate.
Next, the hospital wanted its 96-bed NICU on the fourth floor for easy access to labor and delivery below. Additionally, the Texas Department of State Health Services requires that all patients have access to natural light, including the NICU. However, says Tina Larsen, healthcare planner on Parkland and project manager with Corgan (Dallas), “The physical skin of the building wasn’t enough to have that many patient rooms on a floor and get daylight everywhere and make it somewhat efficient for the staff.” So light wells were embedded on the roof of the NICU to bring daylight into interior rooms, and the adjacent ICU tower was built with an offset, where that keyhole appears, allowing light to hit the perimeter of the NICU.
The strategy worked well, as Parkland required only 36-bed floors in the ICU tower, as opposed to the longer med/surg floors in the tower above it, which have 72 beds. There, the length of the tower was extended to accommodate the additional rooms by spanning the 60 feet that create the cantilever, a move that also allowed light into the NICU below and permitted a necessary alignment of an elevator bank.
Another key to the massing was to create a separation between the Women’s and Infants Specialty Health (WISH) tower and the acute care tower so they would be of the same hospital but with distinct identities—and fit on the site. “That’s when the whole idea of taking the bars and rotating them that 90 degrees came along, and then the idea of having the WISH tower span across the entry and connect to the WISH clinic below,” Adams says of the bridge effect created.
In sum, Parkland’s dynamic massing was created. “Once we did all those moves, it was clear that the building itself became an icon, but it really is a simple expression of the function,” says Jim Henry, healthcare designer on the project and design principle at HDR (Dallas), of the strategic internal moves that created the impressive massing. (For details on how the building was constructed by general contractor and construction manager BARA, a joint venture of Balfour Beatty Construction, Austin Commercial, H.J. Russell & Co., and Azteca Enterprises Inc., see “From the Ground Up: New Parkland Hospital.”)
Pieces and parts
Despite the creative solutions found to fit the program on the site as efficiently and functionally as possible, the result will still likely be one of the largest buildings patients or staff will ever enter. “The idea of making 2 million square feet feel accessible was something we started out with from the very beginning: How do you make it easy to navigate and how do you make it feel accessible so it’s not overwhelming? It comes down to this idea of decentralization and breaking it down into smaller, usable components,” Henry says.
For starters, Henry describes, the new Parkland has distinct onstage and offstage zones in both its horizontal and vertical circulation paths. The 72-bed inpatient floors are divided into two 36-bed units and the ICU tower uses a 36-bed unit. The beds are then broken down into two 18-bed groups and three six-bed pods per group, each with its own work and resource areas and staff assigned to just 18 rooms. “Because the building is so large, it creates a neighborhood or zone that you go to every day so you’re not distracted by the fact that this floor is 72 beds long. You’re really focused on this 18-bed zone, and it’s not that big. It’s not intimidating,” Larsen adds.
The building has 45 elevators with separate systems for public, supplies, and patient transport, with the latter two out of site from visitors so there’s no cross use. The building components were then stacked vertically to allow staff easy access to complementary services and limit horizontal travel. For example, surgical inpatient rooms are located above surgery and women’s services are located above labor and delivery and the NICU.
Further, individual departments are designed with a modular approach, breaking square footage down into manageable pieces—a solution used to address the massive 154-exam room ED by separating it into 12-room pods. The same idea is used in radiology, where there are carved-out subcomponents, such as CT, MRI, nuclear, or ultrasound services; the 27-OR surgical block is also divided into sections with prep and recovery spaces dedicated to specific groupings but built with enough flexibility to be reassigned based on volume.
Finished product
The sheer size and level of use of the building played a significant role in how the interior design unfolded, as well, from durability in materials to wayfinding. But first, it needed to be a space that felt appropriate compared to its exterior. “It’s very sleek, very rectilinear, and very modern, which aren’t necessarily themes you find in healthcare interiors. So we had to find a way to not make it feel so different when you come in,” Roelofs says.
Additionally, Parkland wanted a building that would stack up against its private hospital competitors. “We have some pretty high-end hospital systems in this area, and Parkland wanted us to give them a space that competed with that but still met the functionality of a county hospital and a safety-net hospital. So they said, ‘Give us a hospital of choice but make it durable enough for the high volumes we have and the high abuse that we have.’ It was a tall order,” she says.
Plus, not only does Parkland expect more than 1 million patient visits each year, the building also needs to last at least 50 years despite that level of use.
With all of those things in mind, the interiors solutions started with lots of clean lines that were balanced by warm accents created with paint, furniture, and art that add color but can also be easily changed out in the future, if desired. Specifying proper materials became a bit trickier, though. “One of the main things is the wear and tear, so we had to look at materials that are different than what you would use in most hospitals,” says Kathy Harper, vice president of clinical coordination for Parkland Health & Hospital System.
Flooring alone required four rounds of mockups to determine which material would hold up best to the high use, with a rubber option eventually chosen for 875,000 square feet of the building. However, terrazzo was selected for the ED, a durable material that requires little maintenance and allows Parkland to avoid having to shut down an area to address damage.
Parkland was also designed to reach LEED Silver and was recently certified at LEED Gold, requiring selections that were durable and sustainable.
Themes were avoided outside of a nod to the project’s park concept, with oak leaves and cypress leaves embedded in the flooring to serve as a wayfinding tool in the main concourse, one leading to the acute care tower elevator bank (designated in blue) and the other to the women’s services elevator (designated in gold). Those colors are repeated on the patient floors in footboards, marker board glass, and privacy curtains.
Wayfinding overall was a critical piece of the design due to Parkland’s status as a teaching hospital for the University of Texas Southwestern Medical School, bringing new staff into the building regularly, and the fact that more than 100 languages are spoken by its users. “You can’t rely on just a sign. We used a variety of things; it’s a layered concept,” Harper says, adding that the team took cues from airports in how to move a large volume of people through a space by using a central concourse concept with gates, or destinations, off to the sides.
“You want simple moves and you don’t want to make the families and visitors make a lot of turns. The beauty of it is that you can get from the ED in the main entrance to the cafeteria, and you move all along the edge of the building. You’re always oriented and you can always see outside,” Adams says. Roelofs adds that intuitive wayfinding was also achieved through transitions in ceiling color (white for staff areas and brown for public) as well as architectural changes at key moments that indicate a destination area. “It’s easier to find if it looks like you’re supposed to go there,” she says.
For specific interior spaces, the Parkland team sought feedback from numerous professionals and stakeholders to ensure the design was right, including a patient and family advisory committee and nurse liaison team. “I believe you can’t have too much information to get the right answer,” Harper says. “We tried to assimilate the feedback and the information we were getting from everyone, tried to discern what of that got back to our guiding principles and how they fit, and then, to add another layer on, we had to look at what the cost of each one of those was.”
Part of that process was an extensive use of physical mockups that began even before the project broke ground, specifically to ensure that spaces—from an inpatient room to an OR to a trauma elevator cab—were sized properly.
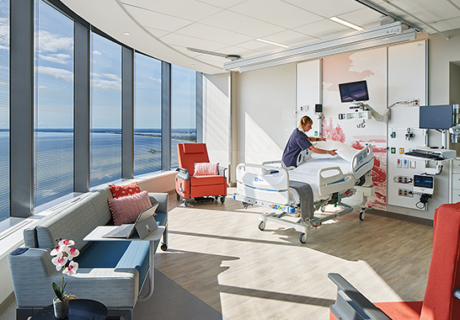
Inpatient rooms, in particular, evolved as the team responded to the feedback that poured in. “The biggest thing with the mockup was not to have just one or two opinions on the space. We had hundreds of staff members come through and make comments,” Roelofs says. The result is rooms that are 360 square feet, acuity-adaptable, and same-handed, with a spacious family zone and outboard toilet room at the footwall. “We had this idea at the beginning that we were designing from the patient room out,” Adams says. “We had to get the patient room right.”
Answering unknowns
As Parkland prepares for an opening in August, the team behind it is realizing a scenario that was anticipated years ago and is now confirmed: Healthcare is changing. “Healthcare reform was just talked about back in 2009-2011, so we were designing a building for the future and we didn’t know what healthcare reform was going to do,” says Lou Saksen, senior vice president, New Parkland construction at Parkland Health & Hospital System. To that end, much of what was designed into the Parkland that stands today was created with the ability to adapt.
For starters, all of the 862 beds aren’t just acuity adaptable but standardized—from ICU to med/surg to labor and delivery, allowing them to be easily reassigned based on need. Parkland’s nine C-section rooms and 27 ORs were built to similar standards, bringing the building’s total invasive surgery space to 36 with the ability to flex either use when necessary. In the ED, 10 Level 1 trauma rooms are built with OR capabilities.
Additionally, Saksen says, at least 100,000 square feet of shelled space was included, largely in the WISH tower but also via individual shelled rooms dispersed throughout the facility to easily adjust to volume changes resulting from reform. The diagnostic and treatment base was also designed with expansion zones where additions can be made. “There was an overall expectation that whatever we did had to be flexible and expandable,” Adams says.
Another key to preparing the building for the unknown was ensuring the infrastructure was in place to support changes in care delivery and operations. “One of our challenges was to set up a backbone to allow whatever was coming in the future to be able to be incorporated. But when you start to think about that over possibly 50 years, it’s incredible,” Larsen says. The building’s ground level offstage area was designed with 16-foot corridors to support a push system for carts and supplies today and a fully robotic transport system later, and floor loads were built to support a higher weight for heavier magnets in MRIs or other larger pieces of equipment down the road.
Then there was technology. “When we were designing this building, the iPad wasn’t here yet. Now everything in the building is going to be driven by an iPad. It’s changing so rapidly, just within the five years that it took to design the building to the point that we installed the technology. So it truly had to be so many things that nobody has a clue of yet,” Larsen says. The building includes plenty of fiber optic cable but is planned to become wireless later, and technology closets are designed to hold one or two server racks today but with a generous amount of square footage to add more.
In patient rooms, headwalls use modular systems where panels can be taken out and technology added, and the footwall features casework that houses a monitor for patient entertainment that can also be used with a Web camera for virtual consultations or eICU observation. “The idea here was that we know the technology in the patient room is going to continue to evolve at a really rapid pace, so we wanted to create a framework so this becomes a technology wall. In a few years, if suddenly there’s a new smart board, we can go in and easily modify that wall without having to cut holes in it or change the infrastructure. It was a flexible approach to how we can adapt technology for the future,” Adams says.
Horizon line
When Parkland began its replacement project, it was guided by the words of the late Dr. Ron Anderson, Parkland’s past president and CEO: The new facility was to be “the hospital of choice, not the hospital of last resort.”
“He recognized that for Parkland to be competitive in this new, evolving healthcare market, it had to be competitive with the private sector and Parkland had to create an environment for patients and families that was on par with that,” Adams says. “It drove so many things,” Harper adds.
The hospital’s overcrowded and outdated care spaces will soon be a thing of the past, as the new Parkland becomes a piece of the system’s overarching goal of addressing the growing Dallas population and community health, with expected pressure on the hospital being reduced through the addition of clinics and outpatient centers (a new med/surg clinic is scheduled to open on the main campus in December 2016). “It’s a comprehensive response, but we had to make sure the building could stand that stress and the need to adapt, certainly for the next 20 years and hopefully further than that,” Saksen says.
Jennifer Kovacs Silvis is executive editor of Healthcare Design. She can be reached at jennifer.silvis@emeraldexpo.com.
To read more about the New Parkland Hospital project, see the following:
- From The Ground Up: New Parkland Hospital
Construction of the New Parkland Hospital in Dallas was a feat unto itself, with a four-party joint venture behind it. From early integration of project team members to prefabrication of building components to figuring out how exactly to build a 60-foot cantilever—and then build on top of it—team leaders share how they brought the project’s 2.1 million square feet to life. - Scale And Scope: New Parkland Hospital
The original program for the New Parkland Hospital was based on a projection a bit smaller than the 2.1 million square feet the hospital ended up with, requiring the project team to make nips and tucks where it could to reel in the budget and deliver what was promised to Dallas County voters—a new hospital. - Rewind: New Parkland Hospital
As the industry awaits the opening of the 2.1 million-square-foot New Parkland Hospital on Aug. 20, here’s a chance to review coverage of the megaproject and hear what its team members had to say over the last seven years, in this look back at Healthcare Design‘s archive.