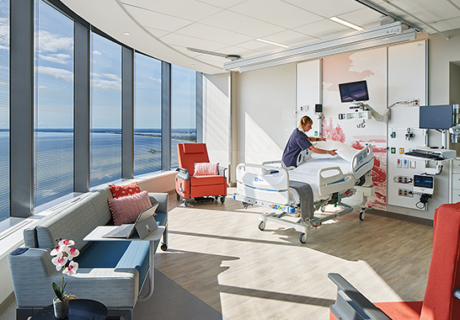
New Mercy Hospital Joplin Is Built "Just In Time"
In the hours and days immediately following the May 22, 2011, EF-5 tornado that devastated Joplin, Mo.—including the former St. John’s Mercy Regional Medical Center—there wasn’t a whole lot of time to think about rebuilding.
“This isn’t something you normally plan for. So we got down there and tried to figure out where we even start with this,” says John Farnen, Mercy’s executive director of strategic projects (St. Louis), who was on the scene following the storm to assess damage to the 800,000-square-foot, 360-bed hospital and secure the site. “When we saw the hospital and how much damage was done to the outside, and the inside was just as bad as the outside, it was just unbelievable.”
While the 1960s structural frame was still standing, most of the windows had been blown out, the roof was torn off, and interior walls had failed. Once patients and staff were evacuated, Farnen and his team got to work removing contents like patient medical records, pharmaceuticals, and IT servers and ensuring that no one could enter the hospital.
Meanwhile, the people of Joplin needed medical care. Mercy set up a triage downtown and tried to identify facilities where patients could be sent afterward, but the other provider in town was soon at capacity, leaving many heading to nearby cities and states. With that immediate need all too apparent, within one week Mercy erected a tent hospital near the existing site. It was later replaced by a prefabricated hospital that allowed Mercy to get through the winter before moving into a modular hospital that opened in early 2012.
But while all of this was happening, Mercy still needed a permanent solution.
Farnen was joined by partners at HKS Inc. and McCarthy Building Cos. Inc., which had worked with Mercy on previous projects and were called upon to help assess the damage. This assessment team, which also included structural, mechanical/electrical, and environmental engineers, went through the building and weighed the options. “It was probably a month or two into assessment before we came to the conclusion that it’s going to cost more to salvage this building and rebuild it than to find a new piece of property and build a new facility,” Farnen says.
Once it was decided to start from scratch on land a few miles away from the old St. John’s, Mercy made a promise to the community that the replacement hospital would be completed by the first quarter of 2015, before the fourth anniversary of the storm. And it was: The new $345 million Mercy Hospital Joplin opened in March.
But for a project of its size—890,000 square feet with 220 patient rooms (with capacity to grow to 260-plus)—making that schedule was a herculean design and construction feat that required the team behind it to pull out all the stops, and then some. “We had to figure out, ‘How do we design and build this in 39 months?’—which is seven months faster than [this team] had ever done it before,” Farnen says.
A combined effort
The team gathered in August 2011 to figure out how the seemingly impossible could be achieved. “The marching orders were already communicated, and then it was up to John [Farnen] to bring the team together and for us in that room to work backwards and figure it out,” says Ryan Felton, McCarthy project director (St. Louis). “There was a lot of push and pull in that meeting, and there were some of us at times who said it’s not possible. And then there was John, keeping the team focused, asking how can we get creative and work through these challenges and still accomplish the end goal.”
A similar project would traditionally require six to eight months in design before starting a fast-track schedule; instead, the design team had just three months, says Norman Morgan, principal-in-charge for HKS (Fort Worth, Texas). The solution was to assign multiple teams to the project. In the midst of construction documents, 51 staff members from HKS alone were dedicated to Mercy Joplin, twice the usual number. McCarthy took the same approach, with 45 of its designers engineering the project at that stage, as well.
Ground was broken in January 2012, and design documents were completed by October of the same year. Ten different bid packages were created to help accomplish the aggressive schedule by anticipating what partners and materials would be needed and in what order to keep the project moving.
And while the tight schedule was partly answered by beginning construction even as design was ongoing, the designers had a head start thanks to a smaller hospital the team was building for Mercy in Springfield, Mo., where new standards were being established for the health system. “A lot of the things that we had started in a smaller model, we basically expanded into this larger plan for Joplin,” Morgan says.
A big piece of that was the design of the diagnostic and treatment areas and how they’re integrated with corresponding clinics on each floor. A concourse runs through the center of the building, the hospital entrance on one side and the clinic entrance on the other. Other standards included sizes for ORs, from a heart room to a hybrid, as well as the general layout for an inpatient floor. Mercy wanted a double corridor for the Joplin site, which, combined with those existing square footages, helped to establish column lines and the width of the building and allowed foundation work to be started early.
The method proved successful, but it didn’t come without anxiety. “I’m putting in columns, yet I haven’t laid out the inside to make sure all the rooms work. We know what our standards are and they should work, but there’s always that worry, because we’re building something before it’s completely designed,” Farnen says.
Case in point: The team was wrapping up final grading on the site at the same time the design of the basement mechanical room was completed and realized that the basement needed to be 4 feet deeper to house the equipment. “Those are the kinds of things we were worried about,” Farnen says. “We’re ahead of the game, but are we going to have to go back and rework the steel that we already put in because it didn’t work? But, honestly, we caught the basement just in time. Everything was just in time.”
In the end, this approach—streamlined by heavy reliance on building information modeling and prefabrication of components such as patient room headwalls and bathrooms as well as mechanical and electrical systems—helped assuage those fears and keep the project on schedule. In fact, there were few design-driven change orders at all and the team was able to bring the project in on time and under budget.
Built to last
With its hospital staff and patients moved from one temporary structure to another after experiencing a tornado of the highest magnitude, another priority at the top of Mercy’s list was making sure that the new hospital had the resiliency necessary to combat a similar event.
To start, the team turned to what it learned in those early days of assessing the existing site. “It was a real case study that we could go back to as we started to design and address certain areas that really failed, like equipment coming off the roof,” Morgan says. Adds Felton, “What withstood [the storm] essentially became the baseline and the standard.”
For example, the assessment showed that large pieces of rooftop equipment, such as air handlers, that were blown off the building during the tornado had actually fallen on more critical pieces of equipment on the ground, including the hospital’s generat
or. A building without air conditioning can be managed, Morgan says, “but when it knocked out the power, we lost everything. As we looked into the new design, it was, ‘How do we anchor that, how do we make sure that if it does fall, it’s not going to hit anything critical on the ground?’”
The solution in this case was to bury the central utility plant. Bunkered and protected underground, it’s also 450 feet away from the hospital. It’s connected by a tunnel to even further prevent the possibility of falling equipment causing a failure in mechanical, electrical, and plumbing systems.
Another major shortcoming at the existing site was the windows. While most of them had failed during the storm, the team noticed that the behavioral health unit, where laminated windows had been installed, held up for the most part.
For the new building, two versions of laminated, high-impact glass were specified: one that could withstand winds up to 250 mph for the intensive care unit (where critically ill patients likely wouldn’t be mobile enough to be moved) and one that could withstand winds up to 140 mph for all other areas. “It took nine months of fabrication and trial and error to get the glass to pass the requirements that we had,” Farnen says.
In terms of what worked at the old hospital, the team found no issues with the structural steel and are confident that today’s more advanced systems can withstand a similar storm, too. And while interior brick and block walls had failed, precast exterior panels survived the blow, inspiring the use of an all-precast skin for the new building. In some areas, brick was laid into precast panels that were hung to achieve a brick look with the same resiliency.
In addition to redundant electric feeds from the north and south, generator capacity to operate for up to 96 hours, battery backups on life support equipment, and interior corridors on all floors that allow patients and staff to move into those spaces and close storm doors to stay protected, another simple yet practical solution was brought to the table.
“When the tornado hit and blew out the glass and blew out the walls, the hallways became cluttered and blocked, and it made it hard to walk and get out,” Morgan says. So the team added a storage closet on each floor of the new hospital where shovels, masks, gloves, and flashlights are readily available to staff in the case of an emergency.
“We’re confident that this building will hold up a whole lot better than the existing facility did. We’re hoping that if we have another event, it won’t shut our doors. We might sustain a little damage, but hopefully we’ll be able to remain open and everybody will be fine,” Farnen says.
Giving back
Over the years that the project team was immersed in bringing the new hospital to life, its members didn’t forget the community that the facility would someday serve and the devastation it had endured. Fundraisers, food collections, and toy drives were held; homes were rebuilt; and plenty of volunteer hours were clocked. In addition, 70 percent of the laborers, vendors, and suppliers on the project were from the area.
In the end, the completion of Mercy Joplin in and of itself is symbolic, a sign of a city rebounding. And being part of that process professionally came with plenty of personal reward. “This is what sparked a lot of energy in the community. To me, for a design professional, this is a once-in-a-lifetime thing to do,” Morgan says. “It was a tragic event, but, at the same time, the end of the project and what we did for the community, the whole team has helped ignite a lot.”
Jennifer Kovacs Silvis is executive editor of Healthcare Design. She can be reached at jennifer.silvis@emeraldexpo.com.
For more coverage of the Mercy Hospital Joplin project, see “Mercy Joplin Provides Care Through Alternative Means.”